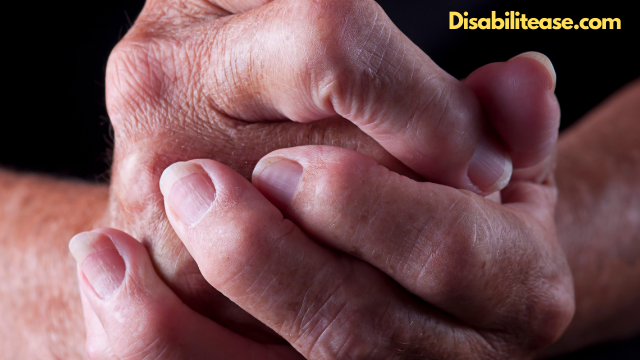
What are Arthritis Bumps? Let’s discuss. Have you ever noticed small nodules on someone’s skin around you, especially an old lady with bumps on her hand?
Have you ever wondered what these are? And you landed on this page because you were just searching for it?
Arthritis bumps are basically nothing but nodules that appear on the skin due to any type of arthritis.
We have a related article for you, you can read 7 Best Arthritis Cream For Hips Reviews Of 2022.
Table of Contents
What Are Arthritis Bumps? Why Are These Bumps Produced?
Whenever there is micro-trauma or friction produced between bones, especially on the hinge or joints part some of the bones are lost in this process.
As a compensatory mechanism, the body tries to recover the loss by growing it back. This growing back process isn’t uniform all the time, producing an irregular surface or a bump.
As a result, these bumps or nodules are produced which can be so small that they are hardly noticeable to be huge.
What Causes These Nodules?
The number one cause is arthritis. While there are many types of arthritis; the main culprits are
- Rheumatoid arthritis
- Osteoarthritis
Rheumatoid Arthritis
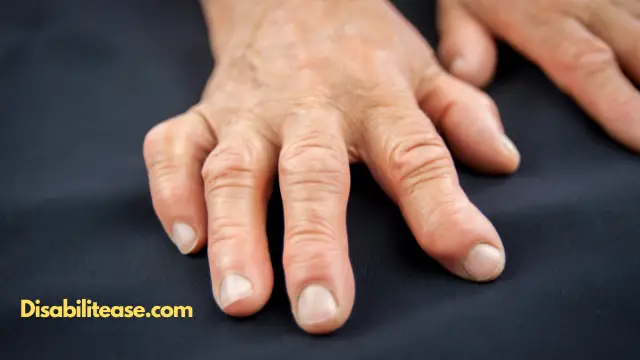
A feature of Rheumatoid arthritis is rheumatoid nodules; which is experienced by around 25% of the population. These nodules are bumps and usually appear on the exposed surfaces, mainly joints like fingers, elbows, and forearms.
Such nodules are mostly compared with pea and walnuts or lemon to describe their size which is they can be minimal and very large too. They may look bad for cosmetic reasons but usually aren’t painful.
However, if they grow on areas like lungs or vocal cords and are larger in size they can result in serious complications like breathing difficulty.
Rheumatoid Nodules
They are aggregates of inflammatory tissue that occur within joints. They are usually circular but can also be in an elongated shape. They can be adherent to underneath tissue, and fascia or mobile and migratory. These nodules can be as small as a pea or as big as a walnut.
What Causes Rheumatoid Nodules?
Less than half of the population that suffers from rheumatoid arthritis develop rheumatoid nodules. Certain factors are thought to increase your chances of developing nodules such as
- Shows up in extreme cases of RA.
- All those who develop nodes are investigated to have high levels of anti-citrulline antibodies.
- Cigarette smoking increases the chance of developing nodules.
- Genetics play a big role in it and increase the chances of occurrence.
- Females are more prone to develop than men.
Risk Factors For Developing Nodules:
- Methotrexate or other arthritis drugs: Methotrexate can induce nodules on the feet, hands, and ears.
- Trauma near joints: nodules are produced usually at pressure points and small joints in case of rheumatoid arthritis and large joints in case of osteoarthritis.
- Exacerbation of Rheumatoid Arthritis: When severity of Rheumatoid arthritis increases one can notice appearance of nodules.
- Smoking: Increases the chances by many folds.
Cure of Rheumatoid Nodules:
Medical treatment:
- Disease modifying anti rheumatic drugs (DMARDS): It slows down the progression of rheumatoid arthritis. Rituximab can decrease the chance of producing nodules.
- Rehabilitation: Physical therapy can be done to combat stiffness, to improve joint flexibility, and reduce pain.
- Analgesics: NSAIDS are given to reduce the pain and anti-inflammatory drugs are given to reduce inflammation of the joints which are the main causative factors.
- Steroid medications:
- In severe cases steroids are used to treat inflammation. Although there may be some side effects when used in the long run, they can be highly effective in treating pain and inflammation.
- Rheumatoid nodules can be injected with corticosteroids like methylprednisolone and it could result in improvement of symptoms but on other side it can cause infection or ulceration of the nodule.
Excision of nodules can be done if they are painful, interfere with daily activities or for cosmetic reason but it should be kept in mind there is no surety that once the nodules are removed they won’t recur ever. They usually return after the surgery.
Osteoarthritis
It’s the most common form of arthritis. It’s a degenerative joint disease that causes wear and tear of joints. Osteoarthritis causes bony nodules at proximal phalanx/joint (Bouchard’s nodes) or at distal joint of finger (Heberden’s nodes).It mostly involves large joints such as hip and knees.
Osteoarthritis most commonly affected parts are:
- Lower back
- neck
- Large weight-bearing joints such as knees, hips, and feet.
Heberden Nodes
There is abnormal bony growth produced as a compensatory response. These nodes are produced to compensate for the bone loss; the new bone growth is abnormal and sticks out as nodes not as ‘Heberden nodes’.
Factors causing formation of Heberden’s Nodes
- Genetic factors: In some families the genes are transmitted and they are seen in generations.
- Any joint already being affected by OA: If a large joint is affected by Osteoarthritis chances of other joints being affected also increases.
- Gout: Erosion and exposure of bones also affects the joints.
- High impact sports: Exercises or sports that are high impact or contain repetitive movements affect joints and increases chance of osteoarthritis.
Treatment
- Herberden’s node currently has no treatment and 100% cure. The medical treatment lies in the management of symptoms of the patient by giving medicines such as:
- NSAIDS and anti-inflammatory drugs given commonly.
- Analgesics: Ibuprofen and paracetamol can be prescribed.
- Codeine can be given because of its strong pain killer properties.
- Topical medications: Capsaicin creams can help relieve pain and inflammation.
- Lifestyle modification: Losing weight can be helpful in putting on extra weight from the joints and preventing further erosion.
- Physical therapy and exercises: This takes down pressure from the affected joints and helps to reduce friction from them. This reduces the chances of formation of further nodules at least.
- Supportive therapies: Hot or ice packs can be used, transcutaneous electrical nerve stimulation (TENS).
- Surgery is not done usually but done in extreme cases and can result in removal of excess bone and the reformation of bone and joint.
Incidence
Incidence of Rheumatoid arthritis and nodules varies worldwide but its rate has been increasing specially in older age groups.
In America 71/100,000 people are diagnosed with rheumatoid arthritis each year.
Hormones play a vital role in preventing and triggering the factors that cause Rheumatoid arthritis. It is seen more in women as compared to men.
A rise is seen at the age of 30 and peaks at 60 in women but later on in men’s life. In the U.S. 3.6% men and 1.7% women are affected annually. However age is no rule to this disease it is also seen in children.
A study conducted in Europe in 2019 showed that Osteoarthritis of Knee joint was 576/100,000 in females and 419/100,000 in males.
Furthermore, Osteoarthritis of hands in women prevailed around 226/100,000and 134/100,000 in men.
Are Nodules Worrisome?
Nodules or bumps on fingers are usually not to be worried until or unless they become painful or hinder daily life activities, put pressure on nerves or are in a sensitive location you can consult a doctor. Its okay to leave them as it is if they cause no problem. However, it may cause trouble to some due to cosmetic reasons and can be treated accordingly.
Summary
Rheumatoid nodules are not a rare complication of rheumatoid arthritis. They usually appear under skin, at joints and rarely develop at vague places internally. Certain modifiable and non-modifiable risk factors play a huge role and can be modified on time to slow down the progress of disease. There is no 100% cure to this disease but the symptoms are manageable.
Heberden nodes are seen in osteoarthritis in which there is wear and tear and erosion of bones and joints that results in formation of nodes. Osteoarthritis cannot be treated fully but managed and improvement of osteoarthritis improves nodules.
Also, make sure to check out my post on BEST Elliptical For Arthritis | Are Ellipticals Good for Arthritis?
Heberden nodes are seen in case of Osteoarthritis mostly and sometimes with gout and Rheumatoid arthritis as well. They can also be managed by medicines and therapies though not 100% cure is there. Underlying causative disease needs to be treated and managed to decrease and slow down the progression.

Hi, my name is Eddie, I am a professional trainer specializing in the elderly population and I’m also a website designer. I love training in the gym, going to the beach, traveling, and having good food.
I combined my love for sport and website designing to make “DisabilitEase” whose purpose is to help elderly and disabled people live a more full and active life, have more fun, and enjoy their unique journey despite any disability.



