Treating osteoporosis in the elderly is an issue that almost every elderly is dealing with, in this article I will help you to understand the disease and how you can avoid it.
This article will show you important information about osteoporosis, which occurs in adults from around the age of 50 – What is the disease? How is it diagnosed? treating osteoporosis in the elderly and can it be prevented?
The information is informative only and does not replace professional medical advice.
Table of Contents
What is osteoporosis
Osteoporosis = bone depletion.
This bone disease is caused by lack of calcium deposits in the body, which causes a decrease in mineral density and damage to the bone structure.
Short explanation: The bone is living tissue, and throughout life, there are processes of decomposition and construction.
Small amounts of bone are destroyed and replaced by a new bone.
During childhood, and especially during adolescence, bone mass is built.
At the end of puberty, between the ages of 20 and 30, you reach the maximum bone mass.
Maximum bone loss varies from person to person.
This amount is determined by genetic factors and environmental factors.
Environmental factors include, among other things, nutrition, physical activity, diseases and various treatments done over the years.
In the third and fourth decades, the bone decomposition rate equals the rate of construction, so that the amount of bone does not change.
Then, especially in postmenopausal women, the rate of bone decay increases the rate of construction, and therefore there is a gradual and continuous decrease in the amount of bone.
The amount of bone in each postmenopausal woman is determined by the maximum bone mass reached at the end of puberty and the rate at which she loses bone mass from entering menopause.
The rate of bone loss is relatively slow: between 1% and a few percents per year.
Over the years, however, it becomes a significant cumulative loss, which is accompanied by changes in bone structure.
The result of these processes is a reduction in bone density and strength and a higher risk of fractures.
The more damaged bones are exposed to fractures.
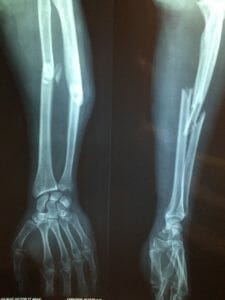
Most of the fractures are in the area of the wrist, thigh, and vertebrae.
The causes of the disease are usually hormonal and especially related to the female hormone estrogen.
This is one of the reasons that postmenopausal women are the primary victims of the disease.
There are other causes of the disease, such as smoking, extreme thinness, chronic diseases, certain medications, and more.
The chances of getting the disease from age 50 and older are about 1 in 3 for women and 1 in 12 for men.
What Causes Osteoporosis?
These are the main risk factors for osteoporosis:
- Sex: Women are at a higher risk than men.
- Age: Adults are at higher risk than young people.
- Body structure: Small, thin people are at greater risk than tall, full-bodied people.
- Heredity: People who have first-degree relatives who have the disease are at greater risk than those who do not have relatives who have the disease.
- Smoking.
- Low exposure to estrogen: Women whose period appeared at a relatively young age and stopped at a relatively young age are more exposed to osteoporosis than women with whom the menstrual cycle occurred at an early age and ended in old age.
- Eating disorders such as anorexia or bulimia and excessive consumption of alcohol and caffeine.
- Various chronic diseases such as chronic arthritis and hyperthyroidism.
- Prolonged use of certain drugs such as steroid drugs (eg prednisone).
- Prolonged lying – for example, due to illness.
How is osteoporosis diagnosed?
Diagnosis of the disease is done by means of a bone density test, which is recommended to be performed from the age of 60 every five years or from age 50 every two years if the patient meets certain criteria (osteoporotic fracture, extreme thinness, osteoporotic fracture of first degree in relatives, Taking certain medications, and more), and is at risk for the disease.
It is better to discover the disease early in order to do a preventive treatment or to relieve the symptoms.
The test itself does not hurt or cause discomfort and is done by a scanner that transmits a stream through the lumbar spine.
The scanner emits a very low amount of radiation that is not hazardous.
If the bone is dense enough, less current will pass. If the bone is not dense enough the current will pass more easily.
The results obtained are relative to the rest of the population in the same sex group and age of the patient:
- Results up to 1 – normal bone density
- A result between 1 and 2.5 – a moderate decrease in bone density called osteopenia
- Outcome over 2.5 – a 25% reduction in bone density indicative of osteoporosis
There is also a higher grade that is considered a difficult condition of osteoporosis in which a patient has already had an osteoporotic fracture.
What are the symptoms?
Osteoporosis develops gradually without being felt because it does not cause any pain.
For this reason, there are those who call it the “silent disease”.
In addition, its main symptom – the tendency to get fractured – may not be discovered for many years simply because the patient has had no accidents.
The bone mass may be reduced by tens of percentage points before fractures occur to diagnose the disease.
The fractures caused by osteoporosis can occur in almost any bone in the body, but they are particularly common in the vertebrae, the wrist, and the femoral neck.
In the vertebrae, the disease can be expressed not only in fractures but also in scoliosis, loss of height, movement restrictions and persistent pain.
The consequences of hip fractures are usually the most severe since they require surgery, hospitalization, and prolonged rehabilitation.
How long does it last?
Osteoporosis cannot be cured.
Once the disease has been diagnosed, it remains for life.
However, the existing treatment can stop or at least slow the further process of calcium depletion and bone depletion.
This implies that the earlier the disease is diagnosed, the more it can be reduced.
Treating Osteoporosis In The Elderly

Treatment for osteoporosis is divided into two parts: preventive treatment and treatment when the disease already exists.
Preventive care (whether at risk, or simply thinking ahead of time) is mainly related to the vitamins and nutrients we consume.
Calcium intake and its high-quality absorption in the body is one of the most important things.
Whether you are getting calcium from dairy products or green vegetables, it is important to make sure that it is well absorbed in your body, because there are other foods that stop the absorption of calcium.
You should consult a dietitian about this.
One of the vitamins that help to absorb calcium is Vitamin D, which is created in our bodies with sun exposure.
Vitamin K is also important for the prevention of osteoporosis and can be obtained by eating green vegetables such as Arabic lettuce, broccoli and etc.
If you are not exposed to nutritional sources, be sure to supplement by taking vitamins.
Another part of the preventive treatment is exercise – walking, bone building exercise, and basically, any type of exercise that puts weight on the bones and skeleton will help delay the disease.
Medications given when the disease is already active in the body are based on taking drugs from two families: drugs that help reduce osteoporosis and bone-building drugs.
In addition to the drugs, the patient should also take calcium supplements and vitamin D.
When there is a significant decrease in bone density, it is also recommended to take medication to prevent osteoporosis.
The main drugs are from the family of bisphosphonates: Faslane, Maxibon, and Alendronate Teva. Bisphosphonates slow the bone decomposition process (“bone absorption” in the doctors’ tongue) and allow for a more effective action of bone-building cells.
Oral bisphosphonates, which might cause gastrointestinal side effects, can be replaced with Aclasta – biphosphonate which is given only once a year.
Another drug to stop osteoporosis is Raloxifene.
It belongs to the group of drugs called SERM – Selective Estrogen Receptor Modulators.
The drugs from this family work on the bone in much the same way estrogen work on the bone: it binds to estrogen receptors and contributes to building the bone. (In contrast, in the breast, they do the opposite: they bind to the estrogen receptor, but do not simulate its action and actually block estrogen absorption.
And there are other new drugs for Treating osteoporosis in the elderly:
Denosumab: This is a biological drug that works in a unique mechanism that inhibits bone breakdown.
The drug is given subcutaneously by a shot twice a year.
Teriparatide: A drug that mimics the activity of the parathyroid hormone and thereby increases bone building rate. The drug is given subcutaneously by a shot daily for two years.
Strontium Ranelate: A new drug to treat osteoporosis given by a dilute powder in a glass of water.
The drug inhibits bone absorption and increases its production.
Strontium is a mineral that mimics to some extent calcium activity in the body and can “clog” holes in the bone when calcium is missing or not absorbed.
Can osteoporosis be prevented?
As mentioned earlier, prevention can be done through diet and exercise.
These actions can reduce the risk of developing the disease.
It is advisable to consult your family doctor about the various prevention options and adapt them to your personal health condition.
In addition, in a meeting with a nutritionist, you will receive an organized menu that will provide you with various options for healthy and nutritious foods containing components that are relevant to the prevention of osteoporosis. With regard to exercise, it is recommended to talk to a physiotherapist who specializes in the elderly and the disease, in order to help you choose the exercises and activities recommended for you.
I hope that I helped you to understand prevention and the ways of treating osteoporosis in the elderly

Hi, my name is Eddie, I am a professional trainer specializing in the elderly population and I’m also a website designer. I love training in the gym, going to the beach, traveling, and having good food.
I combined my love for sport and website designing to make “DisabilitEase” whose purpose is to help elderly and disabled people live a more full and active life, have more fun, and enjoy their unique journey despite any disability.



