I saw the amazing change in the life of people who received a prosthetic leg and so I decided to write about different types of prosthetic legs and more important notes about them.
Sometimes life surprises us with unpleasant surprises and we are forced to part with one of our organs.
Also, make sure to check out my post on the Best Shoes for People with Disability in 2022.
This can be due to an accident, infection, necrosis, medical complication, injury during military service, work accident, and many other reasons that may lead to limb amputation.
Prosthetic legs and prosthetic hands with high technology enable the same person to reach a level of functioning almost identical to the level of functioning before the amputation.
Table of Contents
Different Types Of Prosthetic Legs
If the budget is not a problem you can purchase special prosthetics that allow you to perform any action, including competing in Olympic levels both on the ground and in the pool.
For other people, it is possible to settle for a simpler solution that includes prosthetic legs that are designed for a small burden as in the case of pensioners whose activity is minimal.
The prostheses can be installed from different parts of the body and in different lengths, which means that a prosthesis can be placed under the knee, above or through the knee, as well as prosthesis under the pelvis, through the pelvis and the prosthesis of the foot.
The larger prosthetics consist of a number of replaceable parts according to the changing needs of the customer.
A prosthetic leg, or prosthesis, is a mechanical accessory that serves as a substitute for an organ that is missing in a person and partially or fully fulfills the role of the organ.
The prosthesis can be a cosmetic and aesthetic accessory that hides the fact that a limb is missing (as in the case of a glass eye) or as a technology that helps perform the functions of the amputee limb (such as in the case of a hand or prosthetic leg).
Prosthetics are used by humans since ancient times. And as technology improves, so does the effectiveness of prosthetic limbs. Today, prostheses are found able to work in a way that almost perfectly resembles the real limb.
One of the common prostheses is a prosthetic leg that can replace amputation along the thigh or knee itself and along the calf or ankle. A prosthesis is needed by people who lost their legs due to an accident, diabetes, congenital defect, etc.
Different Types Of Prosthetic Legs
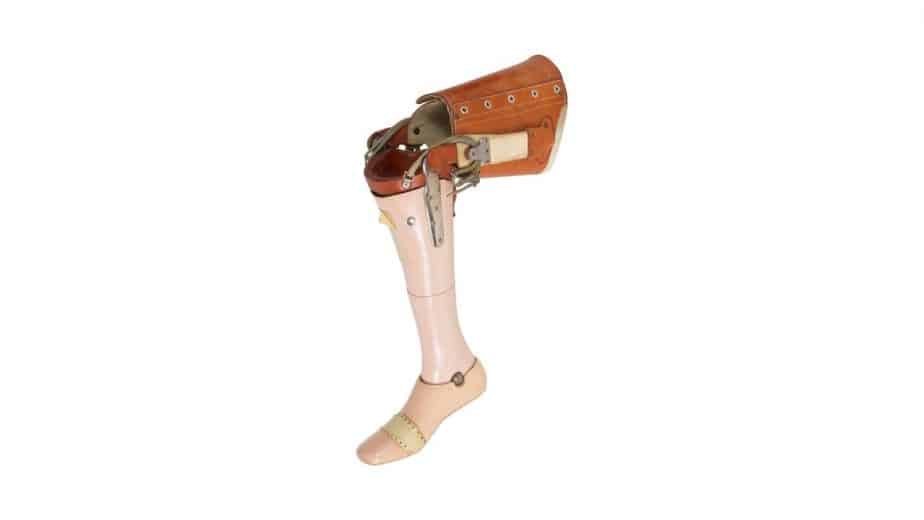
In the prosthetics market there are several types of prosthetic legs adapted to various activities:
- Suitable for walking in an urban environment
- A prosthetic foot for hard terrains (as in Third World countries) – This is a particularly inexpensive prosthetic foot
- A prosthetic foot for athletes – a foot suitable for running and has advanced technology that enables high-intensity activity
- A cosmetic prosthetic foot which is designed to hide the shortage of foot
It is common to divide the prosthetic legs into two groups, above the knee, and below the knee.
Under The Knee Prosthetic Leg
A prosthesis under the knee is intended for use after an amputation done through the Tibia.
This type of prosthesis has different variations and models that have different grip capabilities or are made of various materials.
Prosthesis Above The Knee
A prosthesis above the knee is meant for amputation which done through the femur.
The choice of a prosthesis of this type is very important because its operation requires great effort.
Matching A Prosthetic Leg
Options For Using A Prosthetic Leg To Improve Mobility
When you consider starting to use a prosthesis, it is important that you understand that it is first as to be approved by a doctor.
Before surgery, your doctor will examine your muscle strength, balance, and range of motion.
Before and after the amputation procedure, the doctor, in collaboration with other staff members in your medical care, will assess your general health and closely examine medical problems that may involve additional physical stress and physical injury from diseases such as diabetes that prevent the possibility of using the prosthesis.
In addition, your mental health, energy levels, functionality and resources in your home will also be evaluated for recovery.
If a prosthesis is suitable, the doctor will provide you with a prescription.
The decision to continue with this option or not depends on you.
Assembling A Prosthesis: It’s Not That Simple
If your doctor decides that you are a suitable prosthesis candidate, your first thought is not necessarily related to your preference for a prosthesis, wheelchair, walker or crutches, or if you even want to use a prosthesis.
Before discussing these questions, honestly examine the vital aspects of your life. Think about your values and the quality of your life. Consider your lifestyle, resources, and rehabilitation goals. Sometimes, editing this list of points will help you make the decision.
Next, explore the full range of motion or the options of the available aids for the type of amputation that you had. Consult your medical staff, do research on the web, and consult other amputees.
Keep in mind that some amputees do not use prosthetics at all, and some use them partially.
The questions that you need to ask yourself include the aspects that will help you achieve your goals and allow you to live the life you seek for yourself.
Is there a ramp leading to your home balcony? Do you need a device that will help you return to your workplace or take care of your children? Do you want to move into a custom wheelchair? Is there an elevator instead of stairs to enter the house? Do you intend to drive a car or ride a motorcycle?
“Do I want to be able to walk again?”
This is the question that is supposed to employ amputations. Taking a broader approach to understanding mobility goals will help you. The prostheses technician and physiotherapist will help you choose the mobility device or auxiliary device that will work best for you.
A broader approach will also help you avoid pitfalls after amputation. The main trap is placing unrealistic expectations about your physical abilities. People suffering from lower energy levels and multiple illnesses more than others will find that general mobility after an amputation procedure is more challenging.
However, the use of the implant may be even more intense in terms of energy. A person who has amputated one leg below the knee activates 30 percent more energy during walking with an artificial limb than a person walking on both legs. Walking with a prosthesis above the knee involves a usage of seventy percent more energy.
Is this a scenario you can handle? Do not let your determination circumvent reality. Remember, however, that it’s never too late to improve your physical fitness. Many amputations continue to perform the activities they performed before they were amputated, or they begin new sports activities, such as skiing, golf, and even skydiving.
Benefits Of Using The Prosthesis

If you find that you are a suitable candidate for the prosthesis, but you are not yet sure that this is indeed the right choice for you, consider some of the benefits of using a prosthetic device: In many cases, a prosthetic limb will give you more ability to train and involve in physical activities than other options.
Upward movements help the bloodstream and the digestive system, and studies have shown that amputations who regularly exercise enjoy higher self-confidence and a better general health sense than stationary patients.
The prosthesis gives you increased functional independence. In other words, you may be able to perform many of the activities that you used to do before the loss of the limb, without relying on the assistance of others.
Even aspects that are perceived as marginal, such as independent walking to the bathroom, or independent clothing, are perceived as significant victories.
Leg Amputated people who use prostheses and wheelchairs simultaneously report that they feel less of the stigma of the disabled, wearing a prosthesis.
That is, most amputees who are healthy enough, have access to the prosthesis, use the prosthesis or at least try to use it, are getting great benefits.
The Key To The Success Of The Prosthesis
Ideally, you will work with the same prosthetic specialist for the long-term, so your mutual relationship should be carried out comfortably with the best level of communication.
While your prosthesis specialist needs to know how to listen and communicate well, remember that effective communication is two-sided.
Fill out your part by providing detailed information that the expert needs to work with you successfully.
Establishing a long lasting relationship between you is key to successful use of the prosthesis.
Adjustment process
When choosing the appropriate prosthesis specialist and discussing your personal prescription, lifestyle, needs, and goals, the specialist will examine your stump and begin the adjustment process.
This process can begin with stitches removal, or when it is determined that the stump can carry little weight or cope with stress.
At first, a temporary prosthesis will be used for you, which works as a training wheel.
The temporary prosthetic limb will come about two or three months after the surgery.
The permanent prosthesis will usually come within four to six months after the surgery.
Amputees with health problems, such as diabetes, may wait longer for the adjustment.
The temporary prosthesis will not look like a permanent one, but you can begin to learn to use it under the guidance of your physical therapist.
Prosthetic specialists and some companies create prostheses that will allow you to use the “experimental device” so that you can practice physiotherapy with it and determine if it is suitable for you.
In this scenario, make sure that the trial period is long enough to learn how to get the most out of your device.
Parts of the prosthesis
The type of amputation you have undergone, and the type of prosthesis that is prescribed for you, determine the components from which the prosthesis is produced.
These basic components include the following aspects:
- Chassis. Fits into the stump and connects it to the prosthesis.
It can be customized individually by plaster or fiberglass casting of the stump or can be manufactured according to computerized measurements.
Proper adjustment of the socket is essential for successful use of the implant. When the shape or size of the stump changes due to swelling, sacral degeneration, or body weight fluctuations, the implant may need to be adjusted and re-adjusted. - Sock or sleeve. The interface between the skin and the socket to prevent cuts and friction.
It can consist of fabric, silicone gel or foam, and contain substances that carry anti-contaminant properties. - Holding system. Fixing the prosthesis on the stump.
There are different holding systems, including belts, straps, and ribbons; Anatomical delay; Suspension sleeves; Mechanisms with pin locks; Suction systems and hold system on a vacuum basis.
Each type has advantages and disadvantages, and your choice depends on a number of factors, including cost, aesthetics, lifestyle, type of cutting, level of amputation and goals. - Rod or pylon. Connect the chassis to the external device.
- External device. A hand, a hook, or a device connected to the upper limb end of the prosthesis, to help you perform special tasks.
- Skin cover. A non-mandatory cosmetic cover made up over the prosthesis and designed to look like a natural limb.
The individual components of the level of amputation include the following items:
Foot
prosthesis fit into the following categories:
- Solid ankle, padded heel. A foot with low shock load, providing a natural look with limited movement or no movement at all while walking.
This option is suitable for leg-amputee with function level 1. - Single axis. A foot with low shock load, moving up and down to increase stability.
It allows for stable walking on a variety of surfaces.
This option is suitable for leg-amputee with function level 1. - Multi-axis. A foot with a moderate shock load, moving up and down and side to side.
This option is compatible with amputee with function level 2 or higher. - Dynamic response. A foot with a high shock load that accumulates and releases energy during walking and running. This option is compatible with amputee with function level 3 or higher.
- Multiaxial dynamic response. A foot with a high shock load corresponding to each activity on each surface.
This option is compatible with amputee with function level 3 or higher.
knee
In the event of a leg amputation above the knee, you will need a prosthetic knee.
Knee systems include knee with simple hinges, locked safety knees, heavy hydraulic knees that enable the joint rotation and more expensive knees with advanced technologies controlled by microprocessors and sophisticated software.
There are two basic types of prosthetic knees:
- Mechanical knees. Which serve as a mechanical axis for knee joint replacement.
A locking mechanism, friction, or hydraulic mechanisms are used to control the speed and ease the movement of the knee joint. - Microprocessor-controlled knees. They use a complex computer inside the prosthetic knee, and its function is to monitor and control liquids or air inside the device.
This continuous control enables fast and automatic resistance adjustments, so users can walk at variable speeds and navigate between road obstacles in greater safety.
I hope that now you know more about the different types of prosthetic legs and their components.
If you have any comments, please leave them below.

Hi, my name is Eddie, I am a professional trainer specializing in the elderly population and I’m also a website designer. I love training in the gym, going to the beach, traveling, and having good food.
I combined my love for sport and website designing to make “DisabilitEase” whose purpose is to help elderly and disabled people live a more full and active life, have more fun, and enjoy their unique journey despite any disability.



